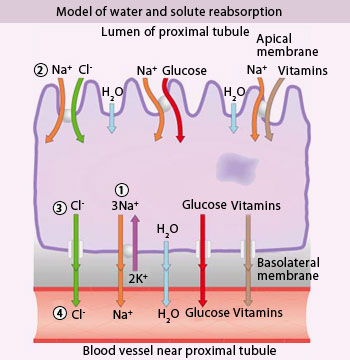
 Model of water and solute reabsorption
Kidney reabsorption ensures the body gets the small molecules it needs back from the filtrate.
Model of water and solute reabsorption
Kidney reabsorption ensures the body gets the small molecules it needs back from the filtrate.
The filtrate passes through the renal tubule where much of the water is reabsorbed together with the useful substances. However reabsorption is limited to the extent that the normal concentration of the blood is not disturbed. The small molecules that the body needs such as ions, glucose and amino acids get reabsorbed from the filtrate back into the blood. Specialized proteins called transporters are located on the membranes of the various cells of the nephron and these transporters grab the small molecules from the filtrate as it flows by them. Each transporter grabs only one or two types of molecules.
For example, glucose is reabsorbed by a transporter that also grabs sodium. Transporters are concentrated in different parts of the nephron. For example, most of the Na transporters are located in the proximal tubule, while fewer ones are spread out through other segments. Some transporters require energy, usually in the form of adenosine
triphosphate which is called active transport, while others are passive. Water gets reabsorbed passively by osmosis in response to the buildup of reabsorbed Na in spaces between the cells that form the walls of the nephron. Other molecules get reabsorbed passively due to solvent drag when they are caught up in the flow of water. Reabsorption of most substances is related to the reabsorption of Na, either directly, via sharing a transporter, or indirectly via solvent drag, which is set up by the reabsorption of Na.
Factors that effect reabsorption: Two major factors which affect the reabsorption process are concentration of small molecules in the filtrate and rate of flow of the filtrate. The higher the concentration of molecules, more molecules can be reabsorbed. Flow rate affects the time available for the transporters to reabsorb molecules. To get an idea of the quantity of reabsorption across the nephron, let’s look at the sodium ion (Na) as an
example:
- Proximal tubule: reabsorbs 65 percent of filtered Na. In addition, the proximal tubule passively reabsorbs about 2/3 of water and most other substances.
- Loop of Henle: reabsorbs 25 percent of filtered Na.
- Distal tubule: reabsorbs 8 percent of filtered Na.
- Collecting duct: reabsorbs the remaining 2 percent only if the hormone aldosterone is present.
Thus, the lumen wall of the epithelial cells of the proximal tubule is like the lumen wall of the small intestine ‐ both are bordered with millions of microvilli to increase surface area. The role of these epithelial cells is to reabsorb ions, nutrients, and water and transport them to the blood vessels nearby.